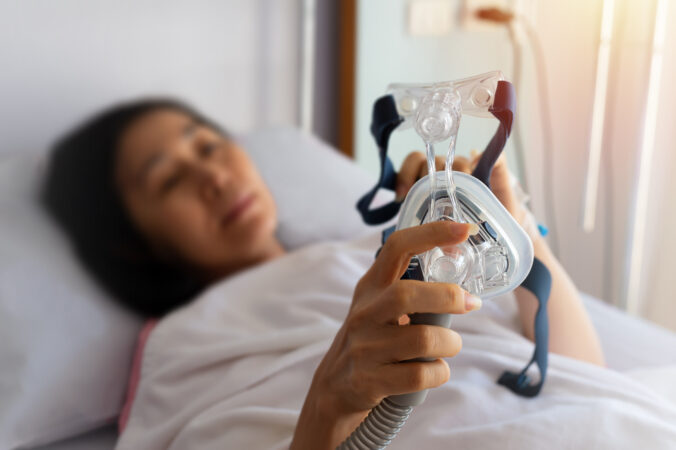
This guide compares clinic and home testing in practical terms, so they can choose the option that fits their situation.
What is a sleep test trying to diagnose?
A sleep test Adelaide service is primarily used to diagnose obstructive sleep apnoea (OSA), a condition where the airway narrows or collapses during sleep. Depending on the type of study performed, it can also help assess central sleep apnoea, periodic limb movement disorder, and certain parasomnias.
The purpose of testing is to measure breathing patterns, oxygen levels, and sleep stages to determine whether symptoms have an underlying medical cause and to assess the severity of the condition.
What happens in a clinic sleep study in Adelaide?
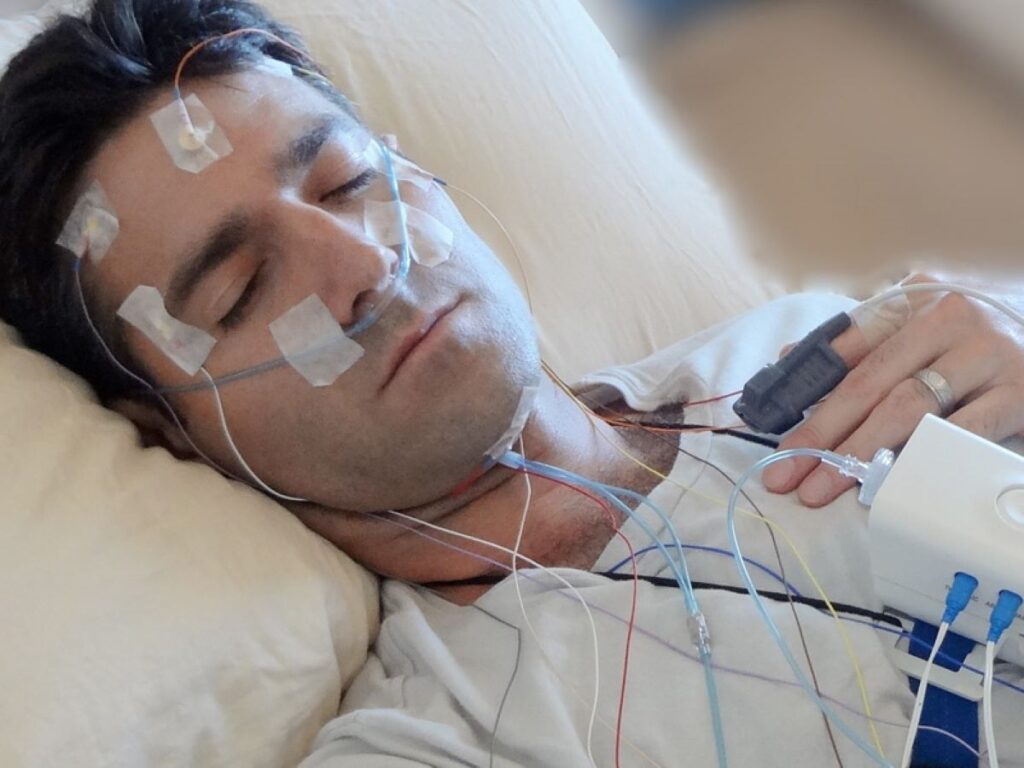
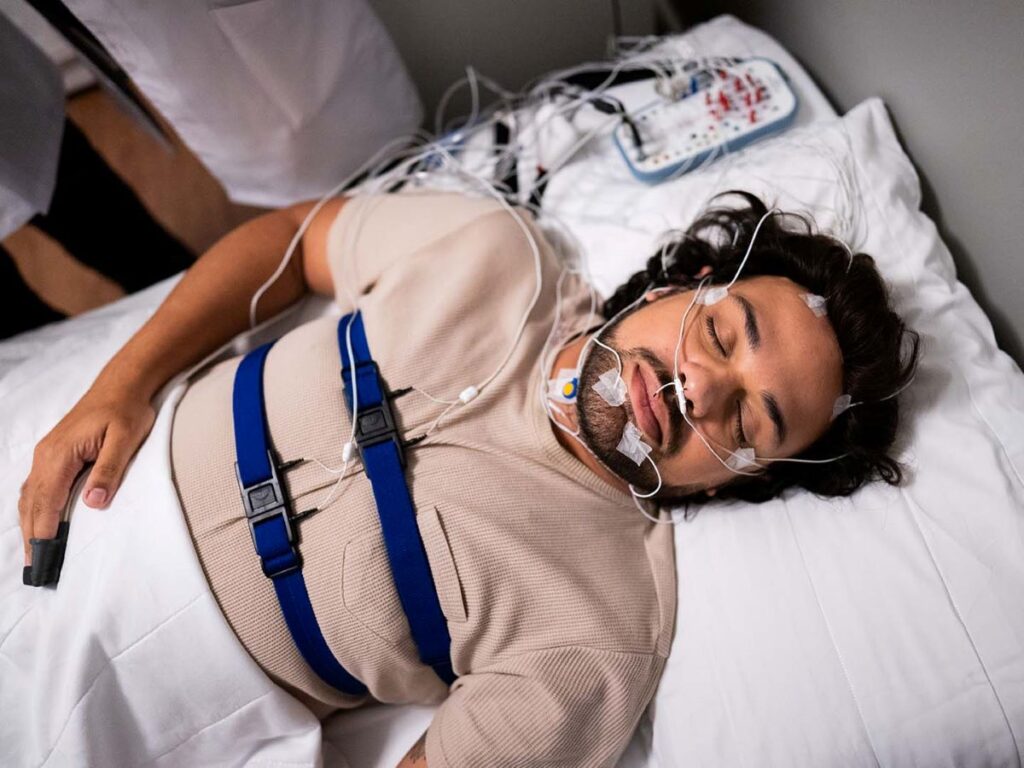
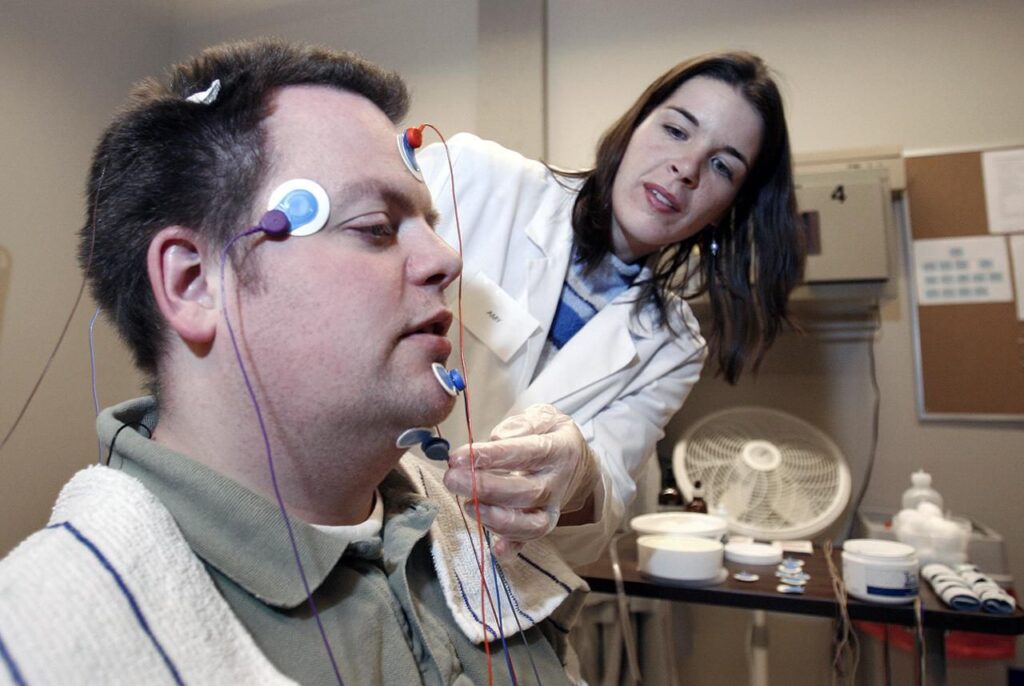
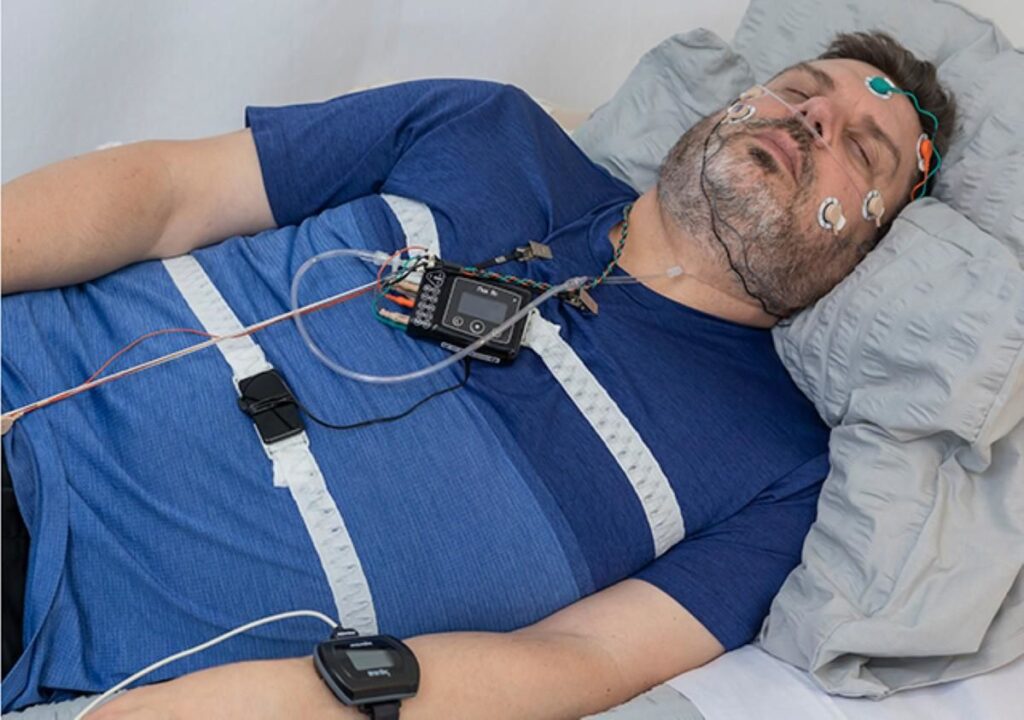
A clinic sleep study (often called an in-lab polysomnography) is done overnight in a sleep clinic or hospital setting. They are fitted with multiple sensors that monitor brain activity, eye movement, muscle tone, breathing effort, airflow, heart rhythm, oxygen saturation and sometimes limb movement.
Because the setup captures a wide range of data, clinic studies can diagnose complex sleep problems and clarify unclear cases. A trained technologist can also adjust sensors overnight, which improves data quality.
What happens in a home sleep test in Adelaide?
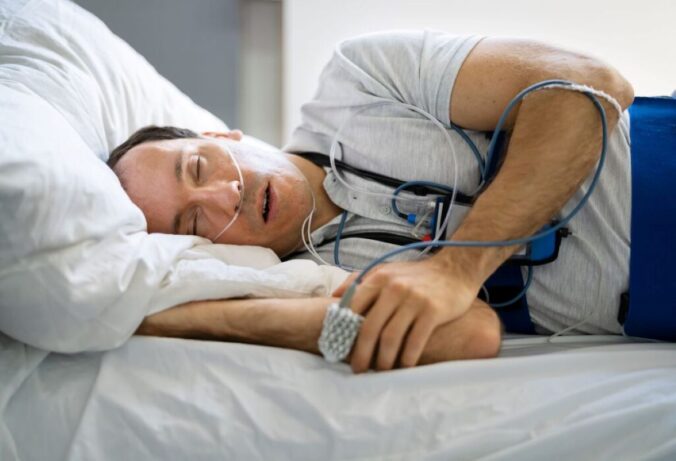
A home sleep test is performed in their own bed using a portable device supplied by a provider. Most home tests measure airflow, breathing effort, oxygen saturation and pulse, and sometimes snoring and body position.
It is typically simpler to set up and more comfortable than a clinic stay. Home tests are commonly used when OSA is strongly suspected and they do not have signs suggesting other sleep disorders.
Which option is more accurate: clinic or home testing?
Clinic testing is generally the most comprehensive and is considered the reference standard for diagnosing sleep disorders. It measures actual sleep stages and can separate “awake time” from “sleep time”, which matters when calculating indices such as the apnoea-hypopnoea index (AHI).
Home testing can be accurate for straightforward, moderate-to-severe OSA, but it may underestimate severity in some people, especially if they have insomnia, fragmented sleep or milder disease.
Who is home testing best suited to?
Home testing often suits people with a high likelihood of obstructive sleep apnoea and relatively uncomplicated health profiles. It can be a practical first step when their main symptoms are loud snoring, witnessed breathing pauses and excessive daytime sleepiness.
It also suits those who sleep poorly outside their own environment, have caregiving responsibilities, or want a quicker, more convenient pathway to an initial diagnosis.
Who is clinic testing best suited to?
Clinic testing is often better when symptoms are complex, risks are higher, or previous testing was inconclusive. It is commonly recommended if they have significant heart or lung disease, suspected central sleep apnoea, neuromuscular conditions, or symptoms that could indicate other disorders.
It can also be preferred when the clinician needs detailed sleep staging data, or when safety and supervision overnight are important.
What are the biggest pros and cons of a clinic sleep study?
A clinic sleep study’s main advantage is depth of data and diagnostic clarity. It can capture sleep stages, arousals and multiple signals that help identify conditions beyond obstructive sleep apnoea.
The main downsides are inconvenience and comfort. Sleeping in a clinic with many sensors can feel unnatural, and availability may involve longer waiting times. Costs can also be higher depending on provider and funding pathways.

What are the biggest pros and cons of a home sleep test?
The biggest advantage of a home sleep test is comfort and convenience. They sleep in their own bed, and the process is usually easier to schedule. It can also be more affordable in many cases.
The main limitation is reduced data. Home tests may miss certain disorders, can fail if sensors are applied incorrectly, and may underestimate severity because they often cannot reliably confirm actual sleep time.
How much do sleep tests cost in Adelaide?
Costs vary widely depending on whether the test is arranged privately, through a hospital service, or with health fund support. Clinic studies often cost more because they involve staffing, specialised equipment and overnight supervision.
Home tests are often cheaper, but pricing depends on inclusions such as consultation fees, reporting, follow-up and whether the device is a basic screening unit or a more advanced system. They should confirm the total cost upfront, including the report and any review appointment.
How long does it take to get results and start treatment?
Home testing can sometimes lead to faster results because it is easier to schedule. Some providers can supply a device quickly, then issue a report after the equipment is returned and data is analysed.
Clinic studies can take longer due to limited beds and scheduling, though result timelines still depend on the clinic’s workflow. In both cases, treatment speed also depends on whether they need further assessment, a CPAP trial, or additional testing to confirm the diagnosis.
Can they get CPAP based on a home sleep test?
In many straightforward cases of obstructive sleep apnoea, a home sleep test report can support starting CPAP therapy. The exact pathway depends on the diagnosing clinician and the provider’s protocols.
Some people may still need a clinic-based CPAP titration study, especially if initial treatment does not relieve symptoms, pressures are difficult to optimise, or there are concerns about complex sleep apnoea.
Other Resources : Changes to Diagnostic Services for Sleep Disorders
What questions should they ask before booking a sleep test in Adelaide?
They should ask what the test can and cannot diagnose, and whether clinic testing is recommended based on their symptoms and medical history. It also helps to ask who interprets the results and whether it is reviewed by a sleep physician.
They should also confirm total costs, what follow-up is included, how long results take, what happens if the test fails, and what treatment support is offered after diagnosis. Check out more about sleep test Sydney: how to choose the right provider.
So, should they choose a clinic sleep study or a home sleep test?
If they likely have uncomplicated obstructive sleep apnoea and want a convenient first step, home testing may be a sensible option. If symptoms are complex, risks are higher, or they need the most detailed assessment, a clinic sleep study is usually the better choice.
The most reliable approach is for them to discuss symptoms and medical history with a GP or sleep clinician first, then match the test type to the clinical question they are trying to answer.
FAQs (Frequently Asked Questions)
What is the primary purpose of a sleep test in Adelaide?
A sleep test in Adelaide is mainly used to diagnose obstructive sleep apnoea (OSA), where the airway narrows or collapses during sleep. It also helps assess other conditions like central sleep apnoea, periodic limb movements, and certain parasomnias depending on the test type, by measuring breathing, oxygen levels, and sleep patterns to confirm symptoms and their severity.
How does a clinic sleep study in Adelaide work?
A clinic sleep study, or in-lab polysomnography, is conducted overnight at a sleep clinic or hospital. Multiple sensors monitor brain activity, eye movement, muscle tone, breathing effort, airflow, heart rhythm, oxygen saturation, and sometimes limb movement. This comprehensive setup allows diagnosis of complex sleep problems with adjustments made overnight by trained technologists to ensure data quality.
What are the advantages of a home sleep test compared to a clinic study?
Home sleep tests offer greater comfort and convenience as they are performed in one’s own bed using portable devices. They are simpler to set up, often more affordable, and suitable for individuals with a high likelihood of uncomplicated obstructive sleep apnoea. Home tests focus on measuring airflow, breathing effort, oxygen saturation, pulse, and sometimes snoring and body position.
Which testing option is more accurate: clinic or home sleep tests?
Clinic testing is generally more accurate and considered the reference standard because it measures actual sleep stages and distinguishes awake time from sleep time. Home testing can be accurate for straightforward moderate-to-severe OSA but may underestimate severity in cases with insomnia, fragmented sleep or milder disease due to less comprehensive data capture.
Who should consider a clinic sleep study over a home test?
Clinic studies are recommended for individuals with complex symptoms, higher risks such as significant heart or lung disease, suspected central sleep apnoea, neuromuscular conditions, or when previous tests were inconclusive. They are preferred when detailed sleep staging data is needed or when overnight supervision for safety is important.
What factors should I consider before choosing between a home sleep test and a clinic study in Adelaide?
You should consider your symptoms complexity, health profile, convenience preferences, cost implications, and diagnostic needs. Home tests suit those with likely uncomplicated obstructive sleep apnoea seeking quick diagnosis at home. Clinic studies provide deeper diagnostic clarity for complex cases but may involve longer wait times and higher costs. Consulting a GP or sleep clinician helps determine the best option based on your medical history.