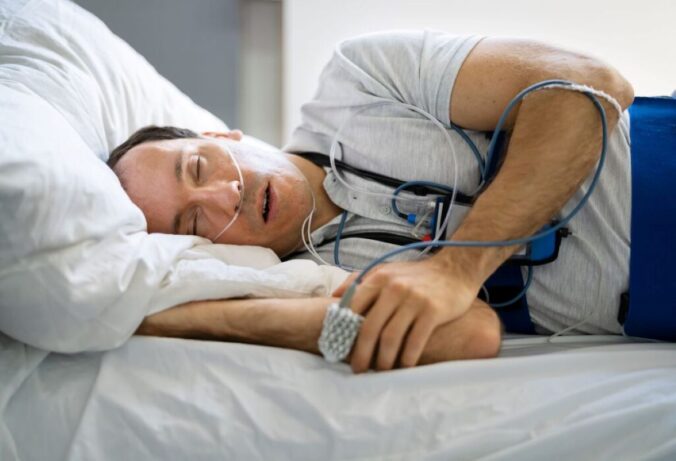
This guide explains how to choose a sleep test provider in Sydney with fewer surprises and a clearer path to treatment.
What is a sleep test, and what does it diagnose?
A sleep test Sydney service measures breathing, oxygen levels, sleep stages, and other signals overnight to help identify sleep disorders. It is most commonly used to diagnose obstructive sleep apnoea (OSA), but depending on the type of test, it can also detect central sleep apnoea, periodic limb movement disorder, and other sleep-related conditions.
The best provider is one that matches the suspected condition with the appropriate test type and then follows through with a clinically appropriate, medically sound management plan.
Should they choose a home sleep test or an in-lab study?
Most people start with a home sleep test when OSA is the main concern and symptoms are straightforward. In-lab studies are usually better when symptoms are complex, when previous testing was inconclusive, or when other disorders are suspected.
A good Sydney provider will clearly explain why they recommend home versus lab. If they push a single option for everyone, it can be a red flag.
How can they tell if a provider is clinically credible?
They should look for medical oversight and clear reporting standards. Ideally, the test is ordered or reviewed by a qualified clinician, and results are interpreted by an appropriately trained sleep physician or specialist team.
A credible provider also supplies a copy of the report, explains the findings in plain English, and outlines next steps rather than leaving patients to guess what to do.
What questions should they ask before booking?
They should ask what the test includes, who interprets it, and what happens after results. They also need clarity on total costs, timelines, and whether follow-up is included.
Useful questions include: how many channels the home test records, whether results include AHI and oxygen desaturation data, and whether a consultation is part of the package. If answers are vague, it’s worth shopping around.
How do referrals work in Sydney, and do they need a GP?
Some providers require a GP referral, while others can organise assessment pathways directly, depending on the service model. A referral can also help with Medicare rebates in certain cases, particularly for specialist consultations and in-lab studies.
If they already have a regular GP, it’s often sensible to involve them. It creates continuity, helps rule out other causes of fatigue, and supports ongoing management. You may like to visit https://hematologyjournal.net/sleep-test-adelaide-clinic-vs-home-testing-compared/ to check out more about sleep test Adelaide: clinic vs home testing compared.
What costs should they expect, and what affects pricing?
Pricing depends on whether it’s a home test or lab study, whether a specialist consult is included, and whether there are rebates or private health cover benefits. Home studies are typically cheaper, but cheap options can become expensive if they don’t include interpretation, follow-up, or a valid pathway to treatment.
They should request an itemised quote. The “real” cost is the full journey from testing to treatment, not just the device dropped at the door.
How fast should they get results, and what is a reasonable timeline?
A common benchmark is a few days to around two weeks from test night to reviewed results, depending on demand and clinical workflow. Some providers offer faster turnaround, but speed should not come at the expense of proper scoring and interpretation.
They should also check appointment availability for follow-up. Fast testing is less helpful if treatment discussions are delayed for weeks afterwards.
What should a good report and consultation include?
A strong report should include the key metrics and be easy to understand. For suspected OSA, that usually means AHI, oxygen saturation trends, time spent below key oxygen thresholds, and positional or REM-related patterns if measured.
The consultation should connect results to symptoms and risk, then recommend realistic next steps. They should feel they understand the “why”, not just the numbers.
Other Resources : Physiology, Sleep Stages – StatPearls – NCBI Bookshelf
How do they avoid conflicts of interest with CPAP sales?
Some providers both diagnose and sell CPAP equipment, which is not automatically a problem, but it can influence recommendations. A trustworthy provider explains multiple treatment options and justifies why CPAP is suggested, especially for mild cases.
They should ask whether they can take the report elsewhere if they want. If a provider resists sharing results or pressures them into buying equipment immediately, it’s a concern.
What treatment support should they expect after the test?
The best providers offer a pathway, not just a diagnosis. That might include CPAP trials and fitting support, mask coaching, troubleshooting, and follow-up checks to confirm therapy is working.
They should also discuss alternatives when appropriate, such as weight management support, positional therapy, oral appliances via a qualified dentist, or ENT review for anatomical contributors. The right provider helps them choose what they can actually stick with.
How should they choose based on their symptoms and health risks?
If they have loud snoring, witnessed pauses in breathing, morning headaches, or excessive daytime sleepiness, a provider experienced in OSA pathways is usually the priority. If they also have heart disease, stroke risk, significant lung disease, or suspected central sleep apnoea, they may need a higher level of specialist oversight and potentially an in-lab study.
They should pick a provider that is comfortable managing complexity. One-size-fits-all testing often misses important details.
What red flags suggest they should choose a different provider?
They should be cautious if pricing is unclear, reports are not shared, or results are not clinician-reviewed. Poor communication, limited follow-up options, and pressure to buy equipment quickly are also common warning signs.
Another red flag is a provider that does not screen properly before testing. Basic screening questions about symptoms, medications, and comorbidities are part of safe care.
How can they make the final decision confidently?
They should shortlist two or three Sydney providers and compare them on clinical oversight, transparency, turnaround time, and follow-up support. The best choice is usually the one that explains the process clearly, provides a complete pathway, and treats them like a patient rather than a transaction.
If they want one simple rule: they should prioritise quality interpretation and aftercare over the cheapest upfront test. A sleep test only matters if it leads to better sleep and better health.
FAQs (Frequently Asked Questions)
What is a sleep test and which sleep disorders can it diagnose?
A sleep test measures breathing, oxygen levels, sleep stages, and other signals overnight to identify sleep disorders. It is most commonly used to diagnose obstructive sleep apnoea (OSA) but can also detect central sleep apnoea, periodic limb movements, and other conditions depending on the test type.
Should I choose a home sleep test or an in-lab study in Sydney?
Most people start with a home sleep test when OSA is the main concern and symptoms are straightforward. In-lab studies are usually better for complex symptoms, inconclusive previous tests, or suspected other disorders. A reputable Sydney provider will explain clearly why they recommend one option over the other.
How can I ensure my chosen sleep test provider in Sydney is clinically credible?
Look for providers with medical oversight where tests are ordered or reviewed by qualified clinicians. Results should be interpreted by trained sleep physicians or specialists. Credible providers supply clear reports, explain findings in plain English, and outline next steps for treatment.
What questions should I ask before booking a sleep test in Sydney?
Ask what the test includes, who interprets the results, what happens after receiving results, total costs, timelines, and if follow-up consultations are included. Inquire about technical details like how many channels the home test records and whether key data such as AHI and oxygen desaturation are reported.
Do I need a GP referral for a sleep test in Sydney and how do referrals work?
Some providers require a GP referral while others organise assessment pathways directly. Referrals can help access Medicare rebates especially for specialist consultations and in-lab studies. Involving your regular GP is often beneficial for continuity of care and ruling out other causes of fatigue.
What costs should I expect for sleep testing in Sydney and what affects pricing?
Costs vary depending on whether you choose a home or lab study, inclusion of specialist consultations, and eligibility for rebates or private health cover. Home studies are generally cheaper but may become costly if interpretation and follow-up aren’t included. Always request an itemised quote covering the full journey from testing to treatment.